
The spine along with the spinal cord and the nerves exiting between the spinal bones perform many essential functions: facilitating brain-body communication, allowing us to stand upright, practice healthy posture, and move flexibly. When the spinal nerves are exposed to uneven pressure, becoming irritated and/or damaged, they have less space to function within, and this is known as radiculopathy and can involve a number of symptoms.
There are 31 pairs of spinal nerves that originate in the spinal cord. These spinal nerves along with the spinal cord partner with the brain to form the central nervous system (CNS). When a spinal nerve is exposed to uneven pressure, it becomes pinched, causing a number of symptoms, and this is known as radiculopathy.
For a better understanding of how the spinal nerves are affected, let’s start by exploring some basic spinal anatomy.
There are a number of spinal conditions/issues a person can develop, and many involve a loss of its healthy curves and alignment.
When a spine is aligned, its vertebrae (bones of the spine) are stacked on top of one another as they were designed to be, and this also means the spine’s natural curves are in place.
The vertebrae have hollow centers and form a type of tunnel, known as the spinal canal, through which the spinal cord passes.
The spinal nerve roots exit the spine, projecting into different areas of the body to form the peripheral nervous system (PNS).
The spine’s natural curves are key to maintaining its overall health; they make it more flexible, better able to absorb mechanical stress, and stronger, like a coiled spring.
There is an intervertebral disc that sits between adjacent vertebrae, and these structures are key to the spine’s overall health, strength, and function.
The discs provide cushioning so adjacent vertebrae don’t rub up against one another during movement, causing friction and excess wear on the spine.
The discs also provide the spine with structural support as adjacent vertebral bodies attach to the intervertebral disc in between, and they also act as the spine’s shock absorbers.
There are three main spinal sections: the cervical spine (neck), thoracic spine (middle/upper back), and the lumbar spine (lower back).
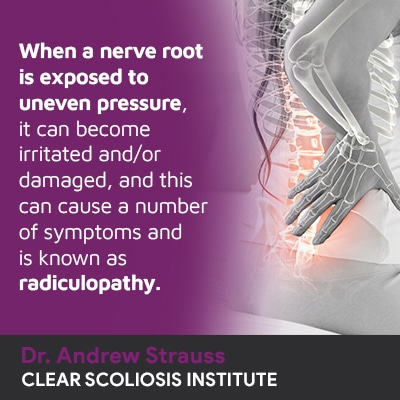
When a nerve root is exposed to uneven pressure, it can become irritated and/or damaged, and this can cause a number of symptoms and is known as radiculopathy.
Symptoms can be felt anywhere along the affected nerve root’s pathway, which can be extensive.
In most cases, the area of the body located closest to the compressed nerve is the most likely to feel its direct effects, but remember, nerves are like tree branches, projecting in multiple directions.
For example, the sciatic nerve, which is the body’s largest nerve, starts in the lumbar spine, so when a spinal condition or issue develops in the lower back, it can cause the sciatic nerve to become irritated, causing sciatic nerve pain.
As the sciatic nerve extends down the back of the buttock, hip, leg, and into the foot, radiculopathy symptoms can be felt throughout the lower body.
As the sciatic nerve is a mixed nerve, containing both motor and sensory fibers, sciatic nerve compression can affect both strength and sensation.
There are a number of radiculopathy causes; some involve spinal injury, and others are caused by the development of spinal conditions, most of which cause changes to the structure of the spine, resulting in a loss of nerve space.
The most common causes of radiculopathy involve a number of issues related to disc degeneration, but additional causes include:

If a disc degenerates, it can become desiccated and change shape, and this can affect the structure of the spine and can introduce uneven pressure to the spine, its surroundings, and nerves within.
Bone spurs are another common cause of radiculopathy, and these are bony overgrowths that develop on the vertebrae, and when there is excess bone in an area of the spine, that excess bone can be encroaching on space needed by the surrounding spinal nerves, causing them to become pinched.
Osteoarthritis is the most common type of arthritis, and when it affects the spine, it weakens the joints and vertebrae, making the spine more vulnerable to injuries, such as compression fractures.
Spondylolisthesis is a condition of spinal instability that involves a vertebral body slipping forward and onto the vertebra below, causing a misaligned spine.
Spinal stenosis is a loss of space within the spine, putting excess pressure on the nerves of the spinal cord.
Subluxations are misalignments of the spinal bones. These misaligments are accompanied by locking or ‘fixation’ of the joints. The exiting nerve root becomes irritated by the abnormal position and restricted movement.
Spinal tumors can also contribute to the development of radiculopathy by pressing on the spine, causing nerve irritation.
In addition, if there is an underlying spinal condition present, such as scoliosis that involves the development of an unnatural spinal curve that also rotates, the spine and its surroundings are vulnerable to the condition’s uneven forces and nerve compression.
While the aforementioned causes don’t comprise a complete list, they are some of the most common causes of radiculopathy, so let’s move on to symptoms of radiculopathy.
Radiculopathy symptoms are shaped by a number of factors, one of which is type; radiculopathy type is determined by its location within the spine, and each type is associated with different symptoms.
In most spinal conditions, the area of the body that’s closest to the affected nerve(s) is going to be the most likely to experience noticeable symptoms and effects.
There are three types of radiculopathy: cervical radiculopathy, thoracic radiculopathy, and lumbar radiculopathy.
Cervical radiculopathy develops in the neck and is diagnosed when a nerve in the area is being compressed.
While symptoms will vary based on severity, some common cervical radiculopathy symptoms can include pain in the neck, shoulders, and upper back, in addition to arm pain, weakness and/or numbness, and a reduced range of motion. In more severe cases the patient will loose dexterity of the hand and tend to drop things.
Thoracic radiculopathy develops in the middle/upper back, the longest spinal section, starting at the base of the neck and extending to the abdomen.
Again, symptoms can vary from patient to patient, but some common thoracic radiculopathy symptoms include chest and torso pain, burning and/or shooting nerve pain felt in the rib cage, down the sides of the body, in the abdomen, and numbness and tingling in the areas most affected.
While each section of the spine is important in its own way, with different roles to play, the lumbar spine has the added responsibility of supporting the weight of the torso and spinal sections above.
The lumbar spine also feels the effects of bending, twisting, and lifting motions, which is why it’s thought that everyone will experience lower back pain at some point in their lives.
When a nerve is compressed and/or irritated in the lumbar spine, a number of symptoms can develop, but most will affect the lower body and tend to get worse during/after extended periods of standing or sitting.
Some common symptoms of lumbar radiculopathy include:
Now that we have explored some common causes and symptoms of radiculopathy, let’s move on to addressing treatment options.
While there are no treatment guarantees, as mentioned, most cases of radiculopathy can be treated non-surgically.
While prescription medications can help with inflammation and short-term pain relief, I want my patients to experience long-term pain relief that’s sustainable, and this is only achieved through proactive treatment that addresses a condition’s underlying cause; otherwise, only symptoms are being addressed, and not the condition itself. As chiropractors, we do not recommend medications.
If disc degeneration is the cause of nerve compression, the focus of treatment is on preserving disc function and preventing further damage by improving the health of the affected disc’s surroundings, which includes nearby nerves.
Lifestyle guidance can also be a part of disc restoration as carrying excess weight, low activity levels, smoking, excessive consumption of alcohol, and repeatedly lifting heavy objects incorrectly can increase the rate of disc degeneration.
Using a variety of therapies to reduce disc bulging, relax associated muscles, and improve core strength is also helpful as a spine that’s surrounded by strong muscles is one that’s going to receive optimal support, taking pressure off the spine, its discs, and nerves.
Improving circulation around an affected disc through gentle stretching and strengthening exercises can help it restore and heal itself; as the spinal discs don’t have their own vascular supply, they absorb nutrients needed for restoration from their surroundings.
Through chiropractic care, including very gentle manual adjustments, a structural change can be worked towards that can also result in less pressure on the affected disc and a change in position that removes pressure from surrounding nerves.
When there is less pressure on the spine and its surroundings, its ability to maintain its natural curves and alignment is improved, and this can help with a number of issues.
When other spinal conditions like stenosis, spondylolisthesis, and/or scoliosis are the cause, these conditions have to drive the design of effective treatment plans, and as they are structural, they have to be primarily impacted on a structural level: through condition-specific chiropractic care. The treatment planning will use all the above modalities in a way that targets the underlying condition.
Radiculopathy has a wide range of severity levels, causes, and symptoms; the most common cause of radiculopathy are disc issues such as degenerative disc disease, bulging, and/or herniated discs.
Just like the rest of the body, the spine is going to degenerate over time, and when that happens, it can also affect the spine’s surroundings and nerves within, and the intervertebral discs are generally the first spinal structures to start deteriorating.
Being diagnosed with radiculopathy means one or more of the spinal nerves are pinched, irritated, inflamed, impinged, and/or compressed.
It’s the nervous system that sends signals to and from the brain and throughout the body, so radiculopathy, depending on the location of the affected nerve(s), can cause a number of different symptoms, including motion and sensory issues.
When it comes to the prevention of radiculopathy, we’re talking about leading a spine-friendly lifestyle that involves maintaining a healthy weight, activity level, practicing good posture, avoiding smoking and excessive alcohol consumption, and understanding the ergonomics of lifting with the legs, and not straining the spine.
As a CLEAR-certified scoliosis chiropractor, I address issues and conditions that affect the spine proactively: by starting treatment as close to the time of diagnosis as possible and combining multiple treatment disciplines, chiropractic care and physical therapy, to customize effective treatment plans.

CLEAR provides a unique and innovative way of understanding scoliosis. Sign up to receive facts and information you won’t find anywhere else.
