
The Scoliosis X-ray is the most common method of diagnosing and monitoring a patient’s scoliosis. Once any underlying pathology or conditions are ruled out, X-rays can tell us what we need to know about a patient’s condition. While many people still have concerns regarding side effects of frequent X-rays, those concerns are unfounded.
Typically, a scoliosis x-ray should be taken from a certain distance; the machine should be 72 inches away from the patient’s body. If the X-ray machine is closer than 72 inches, what can happen is the scoliosis is magnified, making the curve appear slightly larger.
Secondarily, scoliosis X-rays should include the entire spine, meaning from the neck to the pelvis; this is necessary for getting the most accurate images of the spine. Thirdly, the patient should be standing, with arms relaxed, and no shoes on.
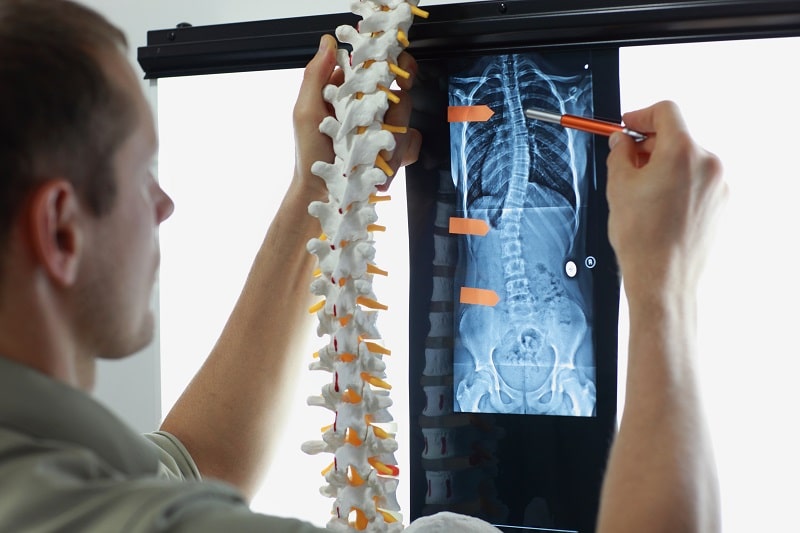
Ultimately, the X-ray should be taking an image of the entire spine all at the same time.
Although X-rays continue to be the most reliable, noninvasive, accessible, and cost-effective method for diagnosing and monitoring scoliosis, there are some common mistakes that can be made.
A lot of times, machines aren’t big enough to take the entire spine, so the images are taken sectionally. There would be one taken of the cervical spine (upper back), another of the thoracic spine (middle back), and one taken of the lumbar spine (lower back).
These images are then stitched together to make a single X-ray image out of the separate images. That stitching process can create an error, which can be very damaging in terms of accuracy.
While it might not seem important whether or not a patient getting a scoliosis X-ray wears shoes, I can assure you it is. The main issue is that shoes can be worn improperly, throwing things off balance, and this can skew the results.
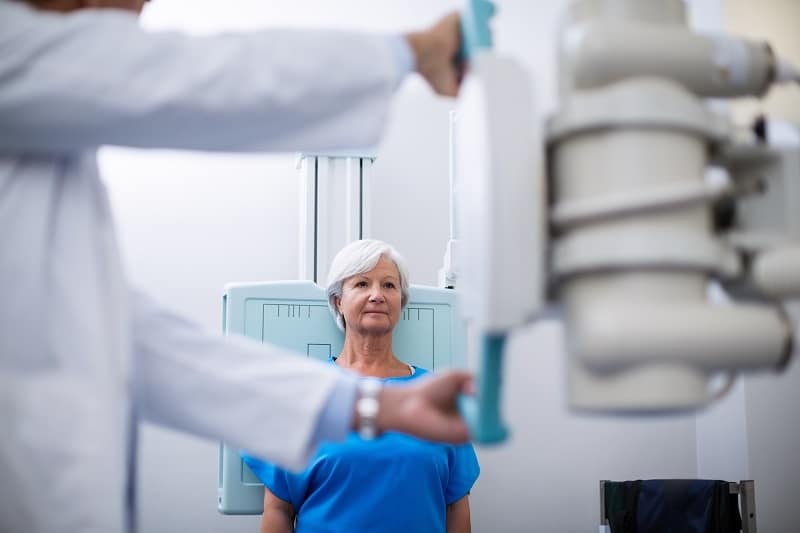
Another common issue that can alter scoliosis X-ray results is the position the patient is in while the X-ray is being taken.
Sometimes, X-rays are taken while a patient is leaning back against the machine. This is not an appropriate position, as it can alter the scoliosis.
Patients with scoliosis often have rib issues where some are farther back on one side and more forward on the other. When a patient leans back, it creates a turn and rotation, and that can lead to a bad X-ray.
I’ve seen scoliosis X-rays that are taken while the patient is lying down; this is horrible for scoliosis X-rays because curves typically reduce when lying down, so X-rays taken from this position won’t give accurate measurements.
Another error can occur if the patient’s arms are not relaxed, or even worse, if they’re purposely positioned symmetrically. This can occur when a patient’s experiencing some type of pain. If the X-ray technician changes the position to make the patient more comfortable, this can alter the presentation of the film.
Typically, scoliosis X-rays should be taken while the patient is in a standing position and from a variety of angles.
A lot of times, when you’re trained to take a scoliosis X-ray, you’re trained to take the most tilted vertebra of the lowest part of the spine and compare it to the most tilted vertebra as you go up the spine. Comparing this tilt to a horizontal level is what gives you the Cobb angle: the most standard measurement for scoliosis.
For example, if L4 is tilted 15 degrees to the left and L1 is tilted 20 degrees to the right, adding those will give you a 35-degree Cobb angle.
However, the most tilted vertebra is a little subjective. Let’s say a patient’s most tilted vertebra is from L4 to T11 and the angle measurement is 50 degrees. If someone else looks and thinks that T9 is the most tilted vertebra and measures from L4 to T9 instead, they’ll get a completely different measurement.
In a scoliosis X-ray, there’s an acceptable error rate of up to 5 degrees from one doctor to another. What that means is if one doctor measures a 50-degree scoliosis and another doctor measures it at 45 degrees without discussing how the measurement was taken, the measurements are considered to be the same because of that 5-degree error rate.
Now, for a doctor that measures their own X-rays and compares and counts the vertebra from the first visit to the next, there should only be a 2-degree error rate; this is because they’re measuring the same film with the same vertebra over and over again.
In terms of getting the most accurate results from a scoliosis X-ray, it’s advantageous to work with the same scoliosis specialist throughout the entire course of treatment.
Not only is a Cobb angle measured from X-rays, other critical information is gathered as well. Coronal balance is another finding used to help determine the best course of treatment; this measurement expresses how the pelvis is vertically aligned to the torso.
If the films are taken correctly, the pelvis should be included. This allows the doctor to assess the Risser Sign. Risser is extremely important for adolescent cases of scoliosis because it helps determine the likelihood of progression due to growth. The Risser scale goes from 0 (full growth potential) to Risser 5 (full skeletal maturity).
A complete and comprehensive set of scoliosis films should also include a Lateral Cobb angle (X-ray taken from the side, not front to back). This lateral Cobb film also gives lots of data regarding how to treat the patient. Variables such as sagittal balance, lumbar lordosis, thoracic kyphosis sacral inclination, and pelvic incidence all come into play.
Also see: Straightening of Lumbar Lordosis
Remember, scoliosis is more than just a bend in the spine; it’s a 3-dimensional problem, so addressing the spine’s sagittal component is a crucial aspect of treatment.
Scoliosis X-rays are taken to determine how the spine is either improving or progressing.
Minimally, during growth, you want X-rays taken every six months and definitely no longer than a year apart. During treatment, scoliosis X-rays happen more often because you’re looking for improvement.
If a patient’s going through treatment, X-rays might be done within a month of each other to make sure the spine is responding to treatment. The last thing a doctor, or a patient, wants to do is go through a bunch of treatment, only to find out it didn’t change anything.
Scoliosis X-ray frequency can vary depending on whether a patient is in active treatment or simply being observed. The danger of solely using observation is when X-rays are taken at fixed time frequencies of, let’s say, every six months, a lot of things can change in those six months.
For parents and caregivers of children with scoliosis, they shouldn’t rely solely on X-rays for observation; they should be instructed on how to check for other signs of progression in between scheduled X-rays such as checking posture and looking for rib and waist issues. This includes being particularly vigilant during signs of growth. This is because growth is the number one reason why scoliosis progresses in children, and unfortunately, it can happen quickly during rapid growth spurts.

For example, let’s say you and your 12-year-old daughter are told to come back in one year. The day after you are told that, your daughter begins a major growth spurt and enters into an aggressive stage of her scoliosis progression. A tremendous amount of progression can happen over that year that could have been prevented.
While there are other signs of progression that can be detected without X-ray, X-ray does remain the most sensitive. Some mild and moderate conditions don’t show any postural signs, but an X-ray can show a curvature as minor as 5 or 10 degrees.
A lot of people have concerns about the potential negative effects of frequent X-rays on children, but those concerns are outdated and unfounded.
There is a lot of data regarding low-dose X-rays and how the risk of any potential negative side effects is extremely low. In fact, lifetime cancer risk increases 0.002% for chest X-rays. New data is actually showing that low-dose X-rays can have a healing effect.
In scoliosis treatment and monitoring, scoliosis X-rays are taken in intervals of 3 to 6 months. This allows for the body to recover and repair.
Ultimately, I wouldn’t worry about getting the minimal amount of X-rays to monitor your scoliosis.
I would worry more about your scoliosis progressing because not enough X-rays are being taken to determine if treatment is working or not.
A scoliosis X-ray remains the most definitive tool for determining the best treatment approach for the patient. The shape and nature of a patient’s scoliosis is going to dictate how they are likely to respond to conservative treatment methods such as exercise, therapy, chiropractic, and bracing.
All these approaches are directly related to what we see on a patient’s scoliosis X-ray. Without a scoliosis X-ray, there is no roadmap for treatment.
In addition to taking a standard set of lateral bending scoliosis X-rays, there are other X-rays that can be used such as sagittal (side view) X-rays used to look at the sagittal profile. These types of X-rays taken while bending to the left and then bending to the right help determine the patient’s level of flexibility in the spine.
The flexibility or rigidity of a patient’s spine is important because it tells us how likely it is that a patient’s going to be able to achieve a reduction.
The stiffer a patient’s spine is on the lateral bending X-rays , the less likely it is that their spine will respond and the more likely it is that the patient will be in need of a more therapeutic approach to improve flexibility.
Scoliosis X-rays can tell us everything we need to know about a patient’s condition. We can measure the degree of their curvature, can see where along the spine the scoliosis is, and can determine how stiff or flexible a patient’s spine is.
These factors are essential in determining the best course of treatment for a patient and how likely it is that their scoliosis will respond to the chosen treatment approach.
While X-rays remain the gold standard for diagnosing, assessing, and monitoring scoliosis, they are still vulnerable to human error. Knowing these areas of vulnerability and how important the correct positioning is can help you advocate for yourself, or a loved one, to ensure the most accurate measurements are being taken.
Without a scoliosis X-ray, there’s no roadmap for a patient’s treatment, which is why here at the CLEAR Scoliosis Institute, we use specialized ‘spot’ X-rays to assess the spine 3-dimensionally.
With an accurate assessment of what’s happening with the entire spine provided by a scoliosis X-ray, our patients have the best possible chance of responding favorably to the chosen treatment approach.
“The author’s views are his or her own and may not reflect the views of CLEAR Scoliosis Institute.”

CLEAR provides a unique and innovative way of understanding scoliosis. Sign up to receive facts and information you won’t find anywhere else.

Do you have offices somewhere that offers treatment? Or offer referrals to like-minded
Practitioners? I live in Maine, alternative medicinal practices are plentiful. Two years ago I was told I have a 30% curve with L3and L4 touching bone to bone. Been through the shots, no dice.
I think the resultant muscle spasms accounts for most of the pain. I last 90 max standing up but resting it works well. I have a dog that keeps me walking daily.
Hi, Alison,
You can find a list of all CLEAR-certified clinics here, and you can search by your location.
Thank you for this information It is very helpful I was told I had Scoliosis In 1980 when I had a x-ray
I had a further x-ray In 1998 which showed the Scoliosis was still there the x-ray doctor said it was
though the Scoliosis was the same an a permanent thing I also have spasmodic torticoliis which I have
had from 1977 after a injury to my neck I had a MRI scan which showed I had two prolapsed discs
and other degenerative changes but said my spine was of normal Alignment It did not say about the
Scoliosis I had a normal x-ray but they did not tell me to take my shoes of and they only x-rayed the
cervical spine not all of the spine, is it possible with the two prolapsed discs happening this could make
the Scoliosis go away, could you email me the information above as I do not have a printer
Hello, John,
Unfortunately prolapsed discs cannot make scoliosis go away. Oftentimes, the prolapsed discs will cause straightening of the cervical spine, which, in turn, can make scoliosis worse.
As far as shoes on or off, only a scoliosis x-ray is taken with shoes off. If they were x-raying the cervical spine. there is no need to remove your shoes. Depending on the severity of the scoliosis, it is rare for it to go away on its own. Scoliosis in its nature is a progressive condition, which means it worsens over time. Typically, this happens at a much slower pace once you are skeletally mature; however, it is not common to have it self correct. In fact, that is very rare.
I would suggest an evaluation with one of our CLEAR Scoliosis Institute certified Doctors to determine the severity of your scoliosis and if you would be a candidate for care in one of our clinics. Our doctors specialize in reducing and stabilizing scoliotic curvatures without the use of surgery. Also, they have specialized equipment in their offices to address the cervical spine disc issues as well. To find the nearest CLEAR Scoliosis Institute certified clinic, please visit our website under Find a Doctor. Please let us know if we can be of further assistance. Best of luck to you.